A Near Catastrophe in the OR Leads to a Solution for Wrong Site Surgery
Dr. Kaveh Khajavi is a board certified neurosurgeon, co-founder and Chief Medical Officer of StartBox.
Over my career, I've gained a fairly broad perspective by working in different hospital settings: military and civilian; academic and private practice; very large medical centers, and small community hospitals. One of the things that always amazes me is how inconsistent safety protocols are from place to place.
The genesis of StartBox is very personal for me. Early in my career, I had a near miss. I nearly performed a catastrophic wrong site surgery on one of my own patients, and it really affected me. At the time, I was serving in the Air Force and was stationed at a very busy hospital supporting both civilian and military trauma. On one particularly busy day, I was performing a very complex cervical spine procedure with another surgeon. A new patient arrived with a head injury, a subdural hematoma, and began rapidly deteriorating. I stayed in the first case as long as possible while they prepared the second one. After being called in, I looked at the films and I looked at the patient and I looked at the OR table. After washing my hands and as I was drying with my towel, I went over to look at the films one more time, I looked back at the patient and I realized with this very sickening feeling in my stomach that the wrong side of the head was shaved, prepped and draped. I was in fact moments away from performing a wrong side craniotomy, which would have had very serious consequences. And so that was the day where I thought to myself: there must be a better way.

Flight Checklist
My career as an Air Force neurosurgeon was driven by my interests in both aviation and medicine. As a young boy, my dream was to be a flight surgeon on the space station. While reality kept me closer to earth, my love for flight, technology and medicine stayed true. In particular, I’ve been fascinated with aviation safety: how can something so dangerous be so safe? Why doesn't an OR run like that? With airplanes, if everybody takes off in a different way, you’re going to a have some serious problems, but with standardization comes efficiency and less room for error. I became a student of aviation safety.
There have been tremendous improvements in aviation safety over the years. In fact, we haven’t had a fatal airline crash in the U.S. since 2009. Airplane crews follow a rigorous process before take-off, and while the pilot is still the captain of the ship, he or she doesn’t act unilaterally. Instead, the crew follows a pre-flight checklist and all members of the crew are encouraged to speak up and halt the flight at anytime. The hierarchy was flattened in order to ensure safety. I became convinced that we had to do this same thing in surgery: we have to make operating on people so routine that when you go to the hospital, you’re at least guaranteed a safe start to the surgery.
Time Out
The Joint Commission Universal Protocol, which includes a surgical time out, was instituted on July 1, 2004. In theory, the surgical time out can be the solution to a lot of the problems in the OR, not just wrong site surgery. But the surgical timeout was rarely performed the same way. In some places the nurse runs it, in some places the doctor leads it. At one hospital they had a bell, like at a deli for pickup. Some ORs post the time out sheet on the board, sometimes it’s on the door, sometimes it’s not in the room at all. On the many occasions that I have worked with another surgeon, I've seen some who perform the surgical timeout with a scalpel already in-hand, letting the nurse go over the surgical checklist. They are passive participants just waiting to get the okay to make the incision.
Surgeon Leadership and Team-Building
The surgeon is traditionally referred to as the captain of the ship in the OR. But in recent years, an increasing amount of unproductive regulation and demands have been placed on surgeons. It’s really challenging to differentiate the wheat from the chaff, what’s important and what’s just bureaucratic distraction. This has created a frustrating environment for surgeons to treat patients. I think the surgeon viewed any efforts to slow him or her down in a negative light. The surgeon didn't want to be questioned and wanted to go in there do the case, do a good job, take care of this patient, and move on to the next procedure. The surgical time out presents an opportunity for the surgeon to step up as the team leader, countering the negative onslaught of bureaucracy. I believe the surgeon shouldn’t be told to do the timeout. The surgeon should lead the timeout, because it's their patient and their team and there are widespread benefits for all in doing so.
After the Universal Protocol was launched, I tried a few things myself. I initially downloaded the timeout sheet from WHO, and sometimes the OR had a large poster-size copy of it on the wall. But I didn't feel like I was getting the buy-in from the rest of the surgical team. We did the job, we went through the checklist, but I didn’t feel there was a lot of teambuilding as a result of it. Over the years, I took more ownership of the checklist and implemented more standardization. We were able to build better teams around that process. Through this, I was able to communicate to the team that pausing to ensure a safe start to every procedure was important. The team saw me not as a surgeon who was just trying to get the most cases finished as possible, but as someone trying to treat this one specific case to the best of my ability, best of our ability. Also, as I took the time to go through the checklist and involved each member of the team, they began to also take ownership of the process. All of us together eliminated ritualized compliance to a potentially bureaucratic process. This paid off. Every once in a while, I might say something wrong and someone would stop me: “You said left side, did you mean right side?”—"You’re correct! I’m sorry, I meant right side.” By providing information for everybody to verify, the team can support me better, each person is enabled to provide constructive input.
A side benefit of this empowerment is that each member of the team gained more job satisfaction, which translated to increased commitment. My surgical technician knows that I’m relying on them, and that I’ve gone over everything and answered any questions they have. Every member of my team knows they’re an integral and valued part of this team and that we do good work together. So, if needed that person is going to stay the late shift, that person is going to delay their lunch because they know I’m in a critical part of the case, which also enhances patient safety… it pays those circular dividends. So, I think my team is a pretty happy team because they feel empowered, appreciated and important, and they feel their job is worthwhile. And enabled because they have information to contribute to patient safety and to better outcomes. All of this starts with good leadership.
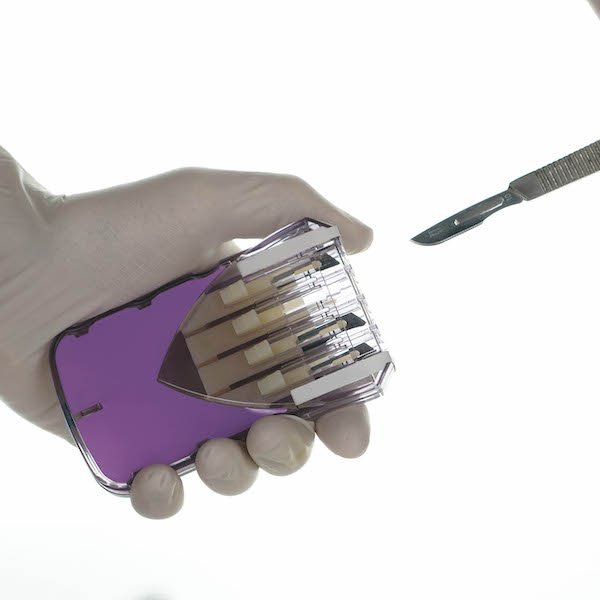
Knife in a Box
As I was applying these concepts of standardization, surgeon leadership and flattening the hierarchy in my OR, I was thinking about how flight crews ensure the compliance with safety procedures. A pilot just can't take off without working through the checklist, there are technological blockers preventing him from doing go. But the surgeon is allowed to say: give me the knife, I’m starting this procedure! And that's when this idea occurred to me: the surgeon should not be given the knife until a proper surgical time out is conducted. Just like the pilot can't take off until the flight checklist has been completed; the surgeon doesn’t get the knife until the surgical checklist is completed.
I developed a simple prototype that showed how you could limit access to the knife by placing it in a locked box. I started thinking of some different things that this box could do, and that's when I came up with the term “start box” because I didn't want people to think this is a “limit box” or a “surgeon limitation box” or “stop box”…it’s a start box: it's a box to help you start your surgery and start surgery safely.
From Ideation to Innovation
After the idea for the box came about, I started working on developing an integrated system around it. That’s when I knew that I needed a good partner to bring it to market. David Lane had been a tremendous support to me in my OR over the years as a medical device distributor. I have always been attracted to innovative technologies to make spine surgery better, and David had already supported my adoption of cutting edge minimally invasive systems. Furthermore, with the common military bond there was an innate sense of trust between us. And so we began to collaborate to develop a comprehensive solution based on proven principles to eliminate wrong site surgery. The StartBox System was developed with a focus on standardizing the start of the procedure in the following way: a clear review of the procedure plan (effective communication/digitization); involving all members of the team (flattening the hierarchy); consistent visual awareness to the procedure laterality (color coding); and only giving the surgeon the knife after confirmation (forcing function).
Start with the Patient in Mind
The most valuable relationship that I have is with my patient, and every member of the healthcare team is there to work with me to deliver the best care possible. The conversation between the surgeon and the patient is the single source of truth, the decision by the patient to undergo a procedure that I’ve recommended. The StartBox System records this interaction, which is then shared with all members of the team throughout the continuum of care, including my clinic staff, the hospital check-in, the preoperative nurses and the OR team. Through this, all members of the team can share in this relationship and be active participants to ensure safety. While other protocols may create artificial and superfluous blockers to patient care, the StartBox System standardizes the way surgery begins. In fact, this standardized process can help cut back on bureaucratic negativity and background noise by focusing on what’s most important. All members of the team can now contribute to effective care and patient safety. And that’s why we talk about StartBox being a comprehensive solution, from decision to incision.
Latest Updates
StartBox Can Reduce Errors to Zero
A study was conducted at a single site over a twelve-month period. Similarly to the experience reported in a peer-reviewed publication, patient harm was prevented and errors were captured. Additionally, a downward trend in near misses was observed, with zero reported during the last five months of the period. This suggests that the StartBox System can help healthcare facilities and providers improve their patient safety and risk profiles over time.
Read More.
StartBox Welcomes Kim Kramer, Head of Risk Consulting
Kim Kramer will lead StartBox in capitalizing on its goals of mitigating risk, reducing medical liability costs and increasing healthcare operational efficiencies.
Read More.
Clinical Experience with StartBox Published in Peer-Reviewed Journal
Innovative Technology System to Prevent Wrong Site Surgery and Capture Near Misses: A Multi-Center Review of 487 Cases
Read More.
Prevent Harm & Reduce CostsStart using the StartBox System in your clinic, surgery center or hospital operating room to track errors and reduce costs today. |

